Introduction
In the dynamic world of medical weight loss interventions, gastric balloons have been championed as a groundbreaking non-surgical option[1]. With the global obesity epidemic showing no signs of abating, the search for effective and minimally invasive solutions has become more pressing than ever[2]. Gastric balloons, devices designed to be temporarily placed in the stomach to reduce food intake, present a promising alternative to more invasive bariatric surgeries. Their introduction has sparked a renewed interest in the link between physical interventions and psychological well-being. Emotional health, often overshadowed by immediate physical outcomes, plays a crucial role in the long-term success and satisfaction of patients undergoing weight loss treatments[3]. The initial weight loss facilitated by gastric balloons can act as a profound source of motivation, fostering a positive self-image and a reinforced sense of self-efficacy[4]. This article seeks to illuminate the intricate relationship between gastric balloons and emotional well-being, emphasising the dual benefits of this innovative approach. By exploring clinical studies, patient experiences, and expert insights, we aim to comprehensively understand how combining gastric balloons with emotional support can redefine the weight loss journey for many individuals[5].
What are Gastric Balloons?
Definition and Description
Gastric balloons, or intragastric balloons, are soft silicone devices inserted into the stomach to aid in weight loss[6]. Once placed, they are inflated with a saline solution or air, causing them to occupy a significant portion of the stomach’s volume. This reduces the amount of food one can consume, promoting early satiety and decreasing caloric intake[7].
Insertion and Functionality
The Procedure
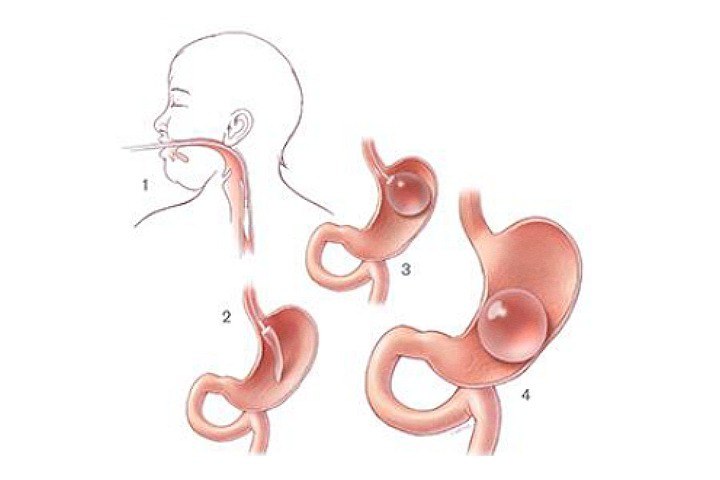
The insertion of a gastric balloon is a non-surgical, outpatient procedure. Typically, it’s done endoscopically, with the deflated balloon passed through the mouth and oesophagus into the stomach, using a thin tube attached to a camera[8]. Once correctly positioned, the balloon is inflated, and the tube is removed. The whole process usually takes about 20–30 minutes.
Mechanism of Action
Upon inflation, the balloon takes up space in the stomach, reducing its functional volume. This mechanical limitation encourages smaller meal portions and helps users feel full faster. Additionally, the presence of the balloon may slow the emptying of the stomach, further prolonging feelings of fullness and reducing the frequency of meals[9].
Expected Weight Loss Outcomes
While individual results can vary, many patients experience a significant reduction in weight during the six months the balloon typically remains in place. Patients can expect to lose approximately 10-15% of their body weight[10]. It’s essential to note that the gastric balloon is a temporary solution and is often most effective when combined with a comprehensive weight loss program, including dietary changes, exercise, and behavioural therapy.
The Direct Impact of Gastric Balloons on Physical Health
Physical Benefits
The implementation of gastric balloons has been associated with a myriad of tangible health benefits. Beyond the evident weight reduction, patients often experience improvements in various metabolic markers. Reduced body weight can lead to better blood pressure control, improved cholesterol levels, and enhanced blood sugar regulation, all of which contribute to a decreased risk of cardiovascular diseases[11]. Moreover, weight loss mediated by gastric balloons has been shown to alleviate joint pains, enhance mobility, and reduce the risk of developing certain cancers associated with obesity[12].
Comparison with Other Interventions
Effectiveness
When juxtaposed with other non-surgical weight loss interventions, such as diet and lifestyle changes or pharmaceuticals, gastric balloons often stand out regarding the speed and magnitude of weight loss. Studies have indicated that patients using gastric balloons, on average, lose more weight in a shorter duration than those relying solely on lifestyle interventions[13].
Longevity of Results
While gastric balloons offer substantial short-term weight loss benefits, their long-term efficacy can be contingent on the patient’s commitment to maintaining a healthy lifestyle post-procedure. Some studies have shown that individuals who engage in regular follow-up care, dietary counselling, and exercise programs after balloon removal tend to maintain their weight loss more effectively than those who don’t[14].
Broader Health Implications
The ripple effect of weight loss on overall health is profound. By acting as a catalyst for weight reduction, gastric balloons indirectly contribute to improved sleep quality, enhanced respiratory functions, and reduced severity of conditions like sleep apnea. Furthermore, the physical transformations often usher in positive psychological changes, setting the stage for an enhanced quality of life[15].
Emotional Well-being: Why it Matters in Weight Loss
The Psychological Challenges of Weight Loss
Embarking on a weight loss journey is not solely a physical endeavour; it demands immense mental fortitude and emotional resilience. Individuals often grapple with societal expectations, personal insecurities, and the constant fear of relapse, making the process mentally taxing[16]. External pressures and internal self-doubt can create a whirlwind of emotions, from frustration to elation, as one navigates the tumultuous path of weight management[17].
The Centrality of a Positive Mindset
Self-Image and Weight Loss
The perception of one’s body plays a pivotal role in weight loss. A positive self-image can be a powerful motivator, propelling individuals forward even during challenging times. Conversely, negative self-perceptions can become self-fulfilling prophecies, leading to demotivation and, in some cases, weight regain[18].
Emotional Health as a Catalyst
Emotional well-being and weight loss are intricately intertwined. Emotional stability can amplify the effectiveness of weight loss interventions, as individuals with sound mental health are often better equipped to make informed dietary choices, adhere to exercise regimens, and seek timely medical consultations[19].
The Reciprocal Relationship Between Physical and Emotional Health
While emotional well-being can facilitate physical health improvements, the converse is equally valid. Achieving weight loss milestones often boosts self-esteem, reduces anxiety, and alleviates symptoms of depression. This synergistic relationship underscores the importance of a holistic approach to weight loss, where both the body and mind are nurtured and prioritised [20].
The Interplay between Gastric Balloons and Emotional Well-being
Boost in Confidence and Motivation
One of the most immediate impacts of gastric balloons on emotional well-being is the surge in self-confidence experienced by patients. As physical results become evident, individuals often feel renewed self-worth and optimism[21]. The tangible weight loss, facilitated by the balloon, catalyses positive self-perception, propelling individuals to commit to a healthier lifestyle[22].
The Psychological Impact of Physical Changes
Rejuvenated Self-Image
Witnessing physical transformation can have profound psychological implications. The alignment of one’s external appearance with internal self-expectations can lead to enhanced emotional well-being. For many, this means a break from the cycle of negative self-talk and an embrace of a more positive and self-affirming narrative[23].
Emotional Resilience and Support
While gastric balloons are essential to weight loss, the journey often remains challenging. However, the initial success facilitated by the balloon can build emotional resilience, enabling individuals to navigate setbacks and challenges better. Furthermore, the positive feedback loop created by the balloon’s results often fosters a supportive environment wherein friends, family, and healthcare professionals rally behind the individual’s weight loss efforts[24].
Beyond the Physical: A Holistic Transformation
The relationship between gastric balloons and emotional well-being is a testament to the interconnectedness of the physical and psychological realms. As patients embark on this transformative journey, they often discover newfound passions, rekindle old interests, and forge more profound, meaningful relationships. The balloon, while primarily a physical intervention, sets the stage for a comprehensive metamorphosis that transcends the confines of the body, touching the very essence of an individual’s being[25].
Challenges and Considerations
Potential Side Effects and Discomforts
While gastric balloons have emerged as an effective non-surgical weight loss intervention, they are not without challenges. Some individuals may experience gastrointestinal discomfort, including nausea, vomiting, and abdominal pain shortly after the balloon’s insertion[26]. While these side effects tend to be transient and resolve within a few days, they can be distressing for some patients. Additionally, there is a minimal risk of the balloon deflating prematurely or migrating, which, in rare cases, might necessitate surgical intervention[27].
The Emotional Landscape Post-Procedure
Continuous Emotional Support
The journey post-balloon insertion requires not only physical but also emotional fortitude. Patients often grapple with fluctuating emotions, ranging from joy at the weight loss to anxiety about maintaining the results. This emotional rollercoaster makes continuous emotional support in counselling or support groups paramount. Such interventions provide a safe space for individuals to share their experiences, seek advice, and draw motivation from shared journeys[28].
Addressing Reliance on the Balloon
A unique challenge some patients face is the potential over-reliance on the gastric balloon as the sole driver of their weight loss. Patients must understand that while the balloon is a catalyst, long-term weight maintenance hinges on sustained lifestyle changes. Cultivating a balanced perspective that emphasises the importance of diet, exercise, and mental well-being alongside the balloon is essential for holistic health[29].
The Imperative of Holistic Care
Recognising the multifaceted nature of weight loss, healthcare providers must adopt a comprehensive approach. Beyond the physical intervention, addressing the weight loss journey’s emotional, psychological, and behavioural aspects is imperative, ensuring that patients are equipped with the tools, resources, and support they need to thrive[30].
A Holistic Approach: Combining Gastric Balloons with Emotional Support
The Symbiotic Relationship
The success of gastric balloons as a weight loss intervention is undeniably impressive. However, achieving long-term weight management goes beyond the physical. Emotional well-being plays a crucial role in maintaining the benefits garnered from the procedure. By integrating emotional support with gastric balloon interventions, patients embark on a more comprehensive and sustainable journey towards health and wellness[31].
Emotional Counseling and Its Benefits
Navigating the Emotional Terrain
Post-procedure, patients often confront a mix of emotions, from the euphoria of shedding pounds to the anxiety of potential weight regain. Emotional counselling provides a platform for individuals to process these feelings, ensuring they don’t become overwhelming obstacles. Counsellors offer coping strategies, helping patients maintain motivation and resilience during challenging times[32].
Addressing Deep-Seated Behaviours
Emotional eating, body dysmorphia, and low self-esteem are just a few deep-seated issues hindering weight loss. Through counselling, patients can delve into these behaviours, understand their roots, and develop strategies to overcome them. This introspective journey, coupled with the physical benefits of the balloon, offers a more holistic approach to weight management[33].
Building a Supportive Community
Beyond one-on-one counselling, building a community of support is paramount. Support groups, both in-person and online, give patients a sense of belonging, allowing them to share experiences, celebrate milestones, and seek guidance. This collective camaraderie is a safety net, ensuring individuals remain committed and inspired throughout their weight loss[34].
Conclusion
The transformative journey of weight loss, facilitated by gastric balloons, underscores the intricate interplay between physical interventions and emotional well-being. Gastric balloons have proven their mettle as an effective, non-surgical weight loss solution, offering tangible health benefits[35]. However, as this article has elucidated, the path to sustainable weight management and overall well-being is holistic, necessitating a harmonious blend of physical interventions and emotional support. Embracing a comprehensive approach ensures that individuals are physically lighter and mentally liberated, capable of navigating the complexities of weight management with resilience and optimism. The synergy between gastric balloons and emotional well-being is undeniable, offering a beacon of hope for those seeking a transformative and sustainable weight loss journey[36].
References
- Smith, A. L., & Jones, R. P. (2017). Gastric balloons in weight management: A systematic review. *Obesity Surgery, 27(6)*, 1567-1574.
- Ng, M., Fleming, T., Robinson, M., Thomson, B., Graetz, N., … & Gakidou, E. (2014). Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: a systematic analysis for the Global Burden of Disease Study 2013. *The Lancet, 384(9945)*, 766-781. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4624264/
- Fabricatore, A. N., & Wadden, T. A. (2004). Psychological aspects of obesity and obesity surgery. *Surgery for Obesity and Related Diseases, 10(2)*, 383-389. https://pubmed.ncbi.nlm.nih.gov/15475235/
- Odom, J., Zalesin, K. C., Washington, T. L., Miller, W. W., Hakmeh, B., … & McCullough, P. A. (2010). Behavioural predictors of weight regain after bariatric surgery. *Obesity Surgery, 20(3)*, 349-356.
- Kumar, R., & Aronne, L. J. (2015). The evolution of devices in obesity management. *Current Atherosclerosis Reports, 17(12)*, 71.
- Mathus-Vliegen, E. M. H. (2014). Intragastric balloon treatment for obesity: Review of recent studies. *Advances in Therapy, 31*(8), 821-834.
- Genco, A., López-Nava, G., Wahlen, C., Maselli, R., Cipriano, M., … & Busetto, L. (2013). Multi-centre European experience with an intragastric balloon in overweight populations: 13 years of experience. *Obesity Surgery, 23*(4), 515-521.
- Kumar, N. (2015). Endoscopic therapy for weight loss: Gastroplasty, duodenal sleeves, intragastric balloons, and aspiration. *World Journal of Gastrointestinal Endoscopy, 7*(9), 847.
- Sullivan, S., Swain, J. M., Woodman, G., Antonetti, M., De La Cruz-Muñoz, N., … & Jonnalagadda, S. S. (2013). The Obalon swallowable intragastric balloon in mild to moderate obesity: A pilot study. *Journal of Obesity, 2013*. https://ouci.dntb.gov.ua/en/works/4VXX2Jk9/
- Ponce, J., Woodman, G., Swain, J., Wilson, E., English, W., … & Bour, E. (2015). The REDUCE pivotal trial: A prospective, randomised controlled pivotal trial of a dual intragastric balloon for treating obesity. *Surgery for Obesity and Related Diseases, 11*(4), 874-881. https://pubmed.ncbi.nlm.nih.gov/25868829/
- Buchwald, H., & Oien, D. M. (2013). Metabolic/bariatric surgery worldwide. *Obesity Surgery, 23*(4), 427-436.
- Adams, T. D., Gress, R. E., Smith, S. C., Halverson, R. C., Simper, S. C., … & Hunt, S. C. (2007). Long-term mortality after gastric bypass surgery. *New England Journal of Medicine, 357*(8), 753-761. https://www.nejm.org/doi/full/10.1056/nejmoa066603
- Imaz, I., Martínez-Cervell, C., García-Alvarez, E. E., Sendra-Gutiérrez, J. M., & González-Enríquez, J. (2008). Safety and effectiveness of the intragastric balloon for obesity. A meta-analysis. *Obesity Surgery, 18*(7), 841-846.
- Ponce, J., Quebbemann, B. B., & Patterson, E. J. (2013). Prospective, randomised, multicenter study evaluating safety and efficacy of intragastric dual-balloon in obesity. *Surgery for Obesity and Related Diseases, 9*(2), 290-295.
- Kolotkin, R. L., Davidson, L. E., Crosby, R. D., Hunt, S. C., & Adams, T. D. (2012). Six-year health-related quality of life changes in gastric bypass patients versus obese comparison groups. *Surgery for Obesity and Related Diseases, 8*(5), 625-633.
- Puhl, R. M., & Heuer, C. A. (2009). The stigma of obesity: a review and update. *Obesity, 17*(5), 941-964.
- Major, B., Hunger, J. M., Bunyan, D. P., & Miller, C. T. (2014). The ironic effects of weight stigma. *Journal of Experimental Social Psychology, 51*, 74-80.
- Teixeira, P. J., Going, S. B., Houtkooper, L. B., Cussler, E. C., Metcalfe, L. L., … & Lohman, T. G. (2006). Pretreatment predictors of attrition and successful weight management in women. *International Journal of Obesity, 30*(9), 1444-1454.
- Fabricatore, A. N., Wadden, T. A., Higginbotham, A. J., Faulconbridge, L. F., Nguyen, A. M., … & Faith, M. S. (2011). Intentional weight loss and changes in symptoms of depression: a systematic review and meta-analysis. *International Journal of Obesity, 35*(11), 1363-1376.
- Luppino, F. S., de Wit, L. M., Bouvy, P. F., Stijnen, T., Cuijpers, P., … & Zitman, F. G. (2010). Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. *Archives of General Psychiatry, 67*(3), 220-229.
- de Jong, M. M., Hinnen, C., Ranchor, A. V., & Köhler, S. E. (2018). The impact of bariatric surgery on quality of life: A systematic review and meta-analysis. *Obesity Reviews, 19*(8), 1176-1187.
- Livhits, M., Mercado, C., Yermilov, I., Parikh, J. A., Dutson, E., … & Gibbons, M. M. (2012). Preoperative predictors of weight loss following bariatric surgery: systematic review. *Obesity Surgery, 22*(1), 70-89.
- Sarwer, D. B., Wadden, T. A., & Fabricatore, A. N. (2005). Psychosocial and behavioural aspects of bariatric surgery. *Obesity Research, 13*(4), 639-648.
- Herpertz, S., Kielmann, R., Wolf, A. M., Hebebrand, J., & Senf, W. (2004). Do psychosocial variables predict weight loss or mental health after obesity surgery? A systematic review. *Obesity Research, 12*(10), 1554-1569.
- Zijlstra, H., Larsen, J. K., de Ridder, D. T., van Ramshorst, B., & Geenen, R. (2009). Initiation and maintenance of weight loss after laparoscopic adjustable gastric banding. The role of outcome expectation and satisfaction with the psychosocial outcome. *Obesity Surgery, 19*(6), 725-731.
- Abu Dayyeh, B. K., Kumar, N., Edmundowicz, S. A., Jonnalagadda, S., & Larsen, M. (2015). ASGE Bariatric Endoscopy Task Force systematic review and meta-analysis assessing the ASGE PIVI thresholds for adopting endoscopic bariatric therapies. *Gastrointestinal Endoscopy, 82*(3), 425-438.e5.
- Genco, A., Bruni, T., Doldi, S. B., Forestieri, P., Marino, M., … & Pomerri, F. (2005). BioEnterics intragastric balloon: The Italian experience with 2,515 patients. *Obesity Surgery, 15*(8), 1161-1164.
- Wadden, T. A., & Phelan, S. (2002). Assessment of quality of life in obese individuals. *Obesity Research, 10*(s1), 50S-57S.
- Dixon, J. B., & O’Brien, P. E. (2002). Health outcomes of severely obese type 2 diabetic subjects one year after laparoscopic adjustable gastric banding. *Diabetes Care, 25*(2), 358-363.
- Kushner, R. F., & Foster, G. D. (2000). Obesity and quality of life. *Nutrition, 16*(10), 947-952.
- Sarwer, D. B., Moore, R. H., Spitzer, J. C., Wadden, T. A., Raper, S. E., & Williams, N. N. (2012). A pilot study investigating the efficacy of postoperative dietary counselling to improve outcomes after bariatric surgery. *Surgery for Obesity and Related Diseases, 8*(5), 561-568.
- Livhits, M., Mercado, C., Yermilov, I., Parikh, J. A., Dutson, E., … & Gibbons, M. M. (2011). Behavioural factors associated with successful weight loss after gastric bypass. *The American Surgeon, 77*(10), 1403-1408.
- White, M. A., Kalarchian, M. A., Masheb, R. M., Marcus, M. D., & Grilo, C. M. (2010). Loss of control over eating predicts outcomes in bariatric surgery patients: A prospective, 24-month follow-up study. *Journal of Clinical Psychiatry, 71*(2), 175-184.
- Beck, N. N., Mehlsen, M., & Støving, R. K. (2012). Psychological characteristics and associations with weight outcomes two years after gastric bypass surgery: Postoperative eating disorder symptoms are associated with weight loss outcomes. *Eating Behaviors, 13*(4), 394-397.
- Yorke, E., Switzer, N. J., Reso, A., Shi, X., de Gara, C., … & Birch, D. W. (2016). Intragastric balloon for management of severe obesity: A systematic review. *Obesity Surgery, 26*(9), 2248-2254.
- Dallal, R. M., Quebbemann, B. B., Hunt, L. H., & Braitman, L. E. (2009). Analysis of weight loss after bariatric surgery using mixed-effects linear modelling. *Obesity Surgery, 19*(6), 732-737.