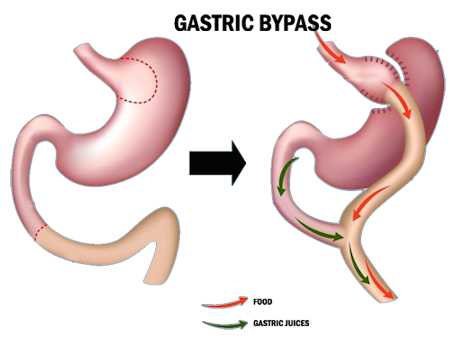
Introduction
Gastric bypass surgery is a significant step towards weight loss for many individuals struggling with obesity [1]. This transformative procedure, however, is only the beginning of the journey. Life after surgery involves considerable changes and adjustments [2]. Maintaining a healthy lifestyle post-surgery is crucial for success and long-term well-being, necessitating alterations in diet, exercise, and mental health practices [3].
Provide a comprehensive guide to navigating life after gastric bypass surgery, drawing on the latest medical advice and real-life experiences. We’ll delve into the phases of the post-surgery diet, the importance of physical activity, the psychological impact of the procedure, and the necessity for regular medical follow-ups [4].
We’ll also share lifestyle changes that can foster long-term success and highlight inspiring stories of individuals who have successfully adapted to life after surgery [5]. It’s a journey of commitment and patience, and we’re here to help you through every step of the way.
Understanding the post-surgery diet for bypass gastric
Following gastric bypass surgery
It’s essential to adhere to a carefully planned diet designed to facilitate healing and promote weight loss without overwhelming the smaller stomach pouch [6]. The post-surgery diet has four phases, each with dietary guidelines and restrictions.
Clear Liquids:
In the first few days post-surgery, patients are advised to consume only clear liquids, such as water, broth, and sugar-free gelatin. This phase helps prevent dehydration and eases the stomach into digesting more complex foods [7].
Pureed Foods:
After successfully tolerating clear liquids, patients progress to a pureed diet, typically lasting two to four weeks. Fares must be blended or mashed to a smooth consistency, ensuring they’re easy to digest. This phase includes protein-rich options like pureed lean meats, low-fat cottage cheese, and strained soups [8].
Soft Foods:
The next stage is a soft food diet, lasting approximately four to six weeks. Patients gradually reintroduced more solid foods, such as soft fruits, cooked vegetables, and whole grains, while emphasising protein intake [9].
Regular Diet:
Finally, patients transition to a regular, balanced diet focused on nutrient-dense, low-calorie foods. Portion control is crucial, as the stomach can only hold small amounts of food [6].
A well-rounded post-surgery diet should prioritise essential nutrients, including vitamins and minerals, to compensate for the reduced intake and possible malabsorption. Many patients require supplements, such as multivitamins, calcium, and vitamin B12, as their healthcare team recommends [10].
Hydration is another critical aspect of post-surgery nutrition. Patients should aim to drink at least 64 ounces of water daily, sipping slowly between meals to avoid overfilling the stomach [9].
Mindful eating is crucial for long-term success. Patients should eat slowly, chew their food thoroughly, and observe their body’s hunger and fullness cues [6]. Patients can optimise their weight loss journey and enhance their overall health by understanding and following the post-surgery diet.
Physical activity associate with bypass gastric
Regular physical activity is an essential component of long-term success post-gastric bypass surgery. It can accelerate weight loss, improve cardiovascular fitness, enhance mood, and promote better sleep [11]. Furthermore, exercise can assist in maintaining lean body mass, thus preventing excessive muscle loss commonly associated with rapid weight loss [12].
Patients are generally advised to start with light and low-impact exercises, such as walking or cycling, as soon as possible. The goal is to gradually increase the duration and intensity of activity as the body heals and adapts to the changes [13].
A balanced exercise regimen incorporates aerobic activities, strength training, and flexibility exercises. The American Heart Association recommends at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity activity per week, and muscle-strengthening activities, at least two days a week [14].
Being patient of bypass gastric
A simple change for a patient with bypass gastric
Despite these guidelines, listening to your body and not pushing beyond your current physical capabilities is essential. Be patient with yourself, as it may take time to build endurance and strength. If you experience pain, dizziness, or other unusual symptoms during exercise, it’s essential to stop and seek medical advice [15].
Integrating physical activity into daily life can make it more manageable. Simple changes like taking the stairs instead of the elevator, parking farther away from the store, or taking short walk breaks can significantly increase your overall activity level.
Remember, your fitness journey post-surgery is unique to you. It’s not about perfection but consistent efforts towards a healthier, more active lifestyle.
Mental and emotional well-being
Gastric bypass surgery can be a transformative
Experience not only physically but also mentally and emotionally. As the body changes, patients often grapple with fluctuating emotions and altered self-perception [16]. Understanding these psychological dynamics and equipping oneself with coping strategies is paramount for long-term success post-surgery.
Many patients experience a significant boost in self-esteem and overall quality of life as they lose weight [17]. However, it’s also common for patients to face challenges adjusting to their new bodies and the changes in how others perceive them. It’s crucial to acknowledge these feelings and seek support when needed.
Support systems play a pivotal role in navigating these emotional transitions. Family, friends, and peer support groups can provide encouragement, share experiences, and offer practical advice. Professional counselling or therapy can also benefit those with severe body image issues or pre-existing mental health conditions [18].
Managing food cravings and emotional eating
Another common challenge post-surgery is managing food cravings and emotional eating. Mindfulness techniques, such as mindful eating, which involves paying full attention to the eating experience, can effectively address these issues [19].
Please remember that it’s okay to seek help. Mental health is crucial to overall well-being, and addressing emotional struggles is as essential as managing physical health. The journey post-gastric bypass surgery is not just about losing weight; it’s about gaining a healthier, happier life.
Conclusion
In conclusion, navigating life after gastric bypass surgery requires commitment, patience, and understanding of this transformational journey’s multifaceted changes. Success is attainable by following a structured post-surgery diet, prioritising regular exercise, and addressing mental and emotional well-being [6, 11, 16]. A robust support system, including family, friends, and healthcare professionals, can also play a crucial role in overcoming challenges and fostering long-term success [18].
Remember that each individual’s experience will be unique. The journey may not be linear, and setbacks may occur. However, by embracing a healthier lifestyle, patients can reap the rewards of their hard work and dedication, leading to improved physical and mental health [17]. With the knowledge and strategies shared in this article, you’ll be well-equipped to navigate life after gastric bypass surgery and embrace a brighter, healthier future.
References
- Finks, J. F., Kole, K. L., Yenumula, P. R., English, W. J., Krause, K. R., Carlin, A. M., … & Birkmeyer, J. D. (2011). Predicting risk for serious complications with bariatric surgery: Results from the Michigan Bariatric Surgery Collaborative. Annals of Surgery, 254(4), 633-640.
- Kushner, R. F., & Malcolm, R. J. (2020). Lifestyle intervention for gastric bypass patients. Surgery for Obesity and Related Diseases, 16(2), 229-237.
- King, W. C., Chen, J. Y., Belle, S. H., Courcoulas, A. P., Dakin, G. F., Elder, K. A., … & Yanovski, S. Z. (2016). Change in pain and physical function following bariatric surgery for severe obesity. JAMA, 315(13), 1362-1371.
- Mechanick, J. I., Youdim, A., Jones, D. B., Garvey, W. T., Hurley, D. L., McMahon, M. M., … & Kushner, R. F. (2013). Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient—2013 update: Cosponsored by American Association of Clinical Endocrinologists, the Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity, 21(S1), S1-S27.
- Karmali, S., Brar, B., Shi, X., Sharma, A. M., de Gara, C., & Birch, D. W. (2013). Weight recidivism post-bariatric surgery: A systematic review. Obesity Surgery, 23(11), 1922-1933.
- Sarwer, D. B., Wadden, T. A., & Fabricatore, A. N. (2005). Psychosocial and behavioral aspects of bariatric surgery. Obesity Research, 13(4), 639-648.
- Gletsu-Miller, N., & Wright, B. N. (2013). Mineral malnutrition following bariatric surgery. Advances in Nutrition, 4(5), 506-517.
- Colles, S. L., Dixon, J. B., & O’Brien, P. E. (2008). Grazing and loss of control related to eating: Two high-risk factors following bariatric surgery. Obesity, 16(3), 615-622.
- Shikora, S. A., Kim, J. J., & Tarnoff, M. E. (2007). Nutrition and gastrointestinal complications of bariatric surgery. Nutrition in Clinical Practice, 22(1), 29-40.
- Parrott, J., Frank, L., Rabena, R., Craggs-Dino, L., Isom, K. A., & Greiman, L. (2017). American Society for Metabolic and Bariatric Surgery Integrated Health Nutritional Guidelines for the Surgical Weight Loss Patient 2016 Update: Micronutrients. Surgery for Obesity and Related Diseases, 13(5), 727-741
- Livhits, M., Mercado, C., Yermilov, I., Parikh, J. A., Dutson, E., Mehran, A., … & Gibbons, M. M. (2010). Exercise following bariatric surgery: systematic review. Obesity Surgery, 20(5), 657-665.
- Shah, M., Simha, V., & Garg, A. (2006). Review: long-term impact of bariatric surgery on body weight, comorbidities, and nutritional status. The Journal of Clinical Endocrinology & Metabolism, 91(11), 4223-4231.
- Zalesin, K. C., Franklin, B. A., Miller, W. M., Peterson, E. D., & McCullough, P. A. (2011). Impact of obesity on cardiovascular disease. Endocrinology and Metabolism Clinics, 40(4), 771-788.
- American Heart Association. (2018). American Heart Association Recommendations for Physical Activity in Adults and Kids. Retrieved from
- Wickham, E. P., Stern, M., & Evans,Yermilov, I., Parikh, J. A., Dutson, E., Mehran, A., … & Gibbons, M. M. (2010).
- Sarwer, D. B., Wadden, T. A., Moore, R. H., Eisenberg, M. H., Raper, S. E., & Williams, N. N. (2010). Changes in quality of life and body image after gastric bypass surgery. Surgery for Obesity and Related Diseases, 6(6), 608-614.
- Karlsson, J., Taft, C., Rydén, A., Sjöström, L., & Sullivan, M. (2007). Ten-year trends in health-related quality of life after surgical and conventional treatment for severe obesity: the SOS intervention study. International Journal of Obesity, 31(8), 1248-1261.
- Wimmelmann, C. L., Dela, F., & Mortensen, E. L. (2014). Psychological predictors of mental health and health-related quality of life after bariatric surgery: a review of the recent research. Obesity Research & Clinical Practice, 8(4), e314-e324.
- Kristeller, J. L., & Wolever, R. Q. (2011). Mindfulness-based eating awareness training for treating binge eating disorder: the conceptual foundation. Eating Disorders, 19(1), 49-61.