The Long-Term Effects and Risks of Gastric Bypass Surgery: Unveiling the Journey to Sustained Weight Loss
Table of Contents
Introduction
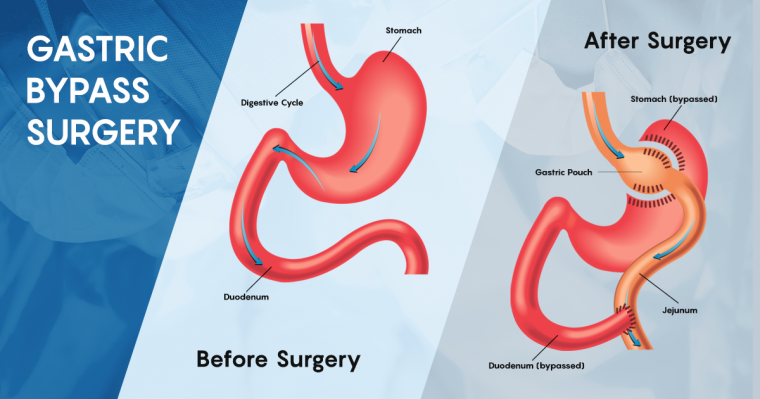
Gastric bypass surgery, a popular bariatric procedure aimed at aiding weight loss in individuals with obesity, has gained significant attention in recent years. Its potential to deliver remarkable short-term outcomes has become an increasingly sought-after intervention. However, as patients embark on this transformative journey, it is crucial to recognise that gastric bypass surgery is not without long-term effects and risks.
Potential health consequences
This article delves into the lasting impact of this surgical procedure on various aspects of patients’ lives and sheds light on potential health consequences. Drawing upon a comprehensive analysis of the existing literature, we aim to explore the physiological, nutritional, and psychological implications of gastric bypass surgery beyond the immediate postoperative period. By understanding the challenges that may arise in the long run, healthcare professionals and patients can make informed decisions and effectively manage the potential risks associated with this weight loss intervention.
Physiological Effects of Gastric Bypass Surgery
Gastric bypass surgery initiates profound physiological changes in the body, leading to sustained weight loss and improvements in various health parameters. Understanding these physiological effects is crucial for comprehending the long-term impact of this surgical intervention.
Weight loss and its impact on overall health:
Gastric bypass surgery results in substantial weight loss, pivotal in reducing obesity-related health risks. Studies have demonstrated significant and sustained weight reduction following the procedure, with a median excess weight loss of 60-70% over several years (1, 2). This weight loss positively affects cardiovascular health, insulin sensitivity, and mortality rates (1, 2).
Changes in metabolic function and hormonal regulation:
Gastric bypass surgery alters the body’s metabolic function and hormonal regulation. It leads to changes in the secretion of various gut hormones, including ghrelin, peptide YY, and glucagon-like peptide 1 (GLP-1) (3). These alterations contribute to decreased appetite, increased satiety, and improved glycemic control (3). The changes in hormonal signalling also impact lipid metabolism, resulting in improved lipid profiles (4).
Potential nutritional deficiencies and malabsorption:
Due to the altered anatomy following gastric bypass surgery, there is a risk of nutritional deficiencies and malabsorption of certain nutrients. Common faults include vitamin B12, iron, calcium, and fat-soluble vitamins (5). Long-term monitoring and appropriate supplementation are necessary to mitigate these deficiencies and maintain optimal health.
Effects on gut microbiota and gastrointestinal function:
Gastric bypass surgery can modulate the composition and function of the gut microbiota. Alterations in gut microbial diversity and abundance have been observed following the procedure, which may contribute to metabolic improvements and weight loss (6). Additionally, changes in gastrointestinal anatomy can affect the digestion and absorption of nutrients, leading to alterations in gut motility and nutrient transit (7).
Long-Term Health Risks and Complications
While gastric bypass surgery has demonstrated significant benefits in weight loss and metabolic improvements, it is essential to acknowledge the potential long-term health risks and complications associated with the procedure. Understanding these risks is crucial for patients and healthcare professionals to ensure comprehensive postoperative care and management.
Increased risk of nutritional deficiencies:
Gastric bypass surgery can lead to long-term nutrient deficiencies due to altered absorption and reduced intake. Deficiencies in essential vitamins, minerals, and micronutrients, such as vitamin B12, folate, iron, calcium, and vitamin D, have been reported (1). Regular monitoring of nutrient levels and appropriate supplementation are essential to prevent deficiencies and their associated health consequences.
Development of metabolic syndrome and related conditions:
While gastric bypass surgery initially improves metabolic parameters, some individuals may develop metabolic syndrome or experience a recurrence of metabolic abnormalities in the long term. This includes insulin resistance, dyslipidemia, hypertension, and glucose dysregulation (2). Long-term follow-up and lifestyle modifications are crucial to mitigate these risks.
Gastrointestinal complications such as ulcers and gallstones:
Gastric bypass surgery can increase the risk of gastrointestinal complications. These may include the development of ulcers, particularly at the anastomosis site, and the formation of gallstones due to rapid weight loss (3). Close monitoring, proper medication, and dietary management are necessary to minimise these complications.
Impact on bone health and risk of osteoporosis:
Gastric bypass surgery has been associated with an increased risk of bone loss and osteoporosis. Reduced nutrient absorption, particularly calcium and vitamin D, and altered hormonal regulation contribute to bone mineral density reduction (4). Adequate calcium and vitamin D supplementation, weight-bearing exercises, and bone health monitoring are essential for long-term skeletal health.
Potential long-term effects on cardiovascular health:
While gastric bypass surgery can improve cardiovascular risk factors initially, the long-term effects on cardiovascular health are still being studied. Some studies suggest that there may be a slight increase in the risk of cardiovascular events in the long term (5). Regular cardiovascular assessments and management of modifiable risk factors remain crucial for patients undergoing gastric bypass surgery.
Psychological and Emotional Effects
Gastric bypass surgery not only impacts the physical aspects of an individual’s life but also has significant psychological and emotional implications. Understanding and addressing these effects are essential for promoting holistic well-being and successful long-term outcomes.
Psychological adjustment to significant weight loss:
Following gastric bypass surgery, individuals experience rapid and significant weight loss, necessitating psychological adjustment. This adjustment process can involve changes in body image perception, self-identity, and self-esteem (1). Supportive counselling and psychological interventions can aid in coping with these changes and promoting a positive body image.
Body image concerns and potential body dysmorphia:
While weight loss after gastric bypass surgery is often desired, body image concerns may persist or intensify. Some individuals may develop body dysmorphia, experiencing distorted perceptions of their appearance despite significant weight loss (2). Body image-focused therapies and support groups can be beneficial in addressing these concerns.
Risk of developing eating disorders or disordered eating patterns:
Gastric bypass surgery can trigger a shift in eating behaviours, which may manifest as disordered eating patterns or even lead to eating disorders such as binge eating or restrictive eating behaviours (3). Close monitoring, nutritional counselling, and psychological support are crucial for early identification and intervention.
Impact on mental health and quality of life:
While gastric bypass surgery can improve the overall quality of life and psychological well-being for many individuals, some may experience challenges with mental health. Common mental health issues following surgery include depression, anxiety, and changes in mood (4). Regular mental health screenings and access to appropriate psychological interventions are essential to address these concerns.
Social and interpersonal effects:
Gastric bypass surgery can influence an individual’s social interactions and relationships. Changes in appearance, dietary restrictions, and altered eating behaviours may impact social gatherings, relationships with family and friends, and social support networks (5). Support groups and counselling can guide managing these social changes and fostering healthy relationships.
Long-Term Success and Factors Influencing Outcomes
The long-term success of gastric bypass surgery relies on various factors, including patient adherence to lifestyle changes, ongoing support, and individual characteristics. Understanding these factors is essential for optimising outcomes and maintaining sustained weight loss.
Factors associated with successful weight maintenance:
Multiple factors influence successful weight maintenance after gastric bypass surgery. Compliance with postoperative dietary guidelines, regular physical activity, and adherence to follow-up appointments play crucial roles (1). Psychological factors such as motivation, self-efficacy, and a positive body image contribute to long-term success (2).
Importance of lifestyle changes and ongoing support:
Adopting and maintaining healthy lifestyle changes is paramount for long-term success. This includes a balanced diet, portion control, regular exercise, and stress management (3). Ongoing support, such as participation in support groups, nutritional counselling, and access to healthcare professionals, can provide guidance and assistance throughout the weight loss journey (4).
Impact of preoperative and postoperative interventions on long-term results:
Preoperative interventions, such as weight loss and psychological assessments, can improve surgical outcomes (5). Postoperative interventions, including nutritional counselling, behavioural therapy, and continued monitoring, support weight maintenance and address potential challenges (6).
Individual characteristics and variability in outcomes:
Individual characteristics, including age, gender, initial weight, and comorbidities, can influence the long-term outcomes of gastric bypass surgery. For instance, younger age and lower preoperative weight are associated with better weight loss maintenance (7). Understanding individual variability and tailoring interventions accordingly can improve overall success rates.
Importance of long-term follow-up care:
Long-term follow-up care is vital to monitor weight loss progress, detect complications, and provide ongoing support. Regular medical assessments, laboratory monitoring, and psychological evaluations ensure comprehensive care and early intervention when needed (8).
Potential Side Effects and Risks
Gastric bypass surgery, like any surgical procedure, carries potential side effects and risks. While the system can be effective in achieving weight loss and improving health outcomes, it is essential to be aware of the possible complications that may arise in the long term.
Surgical complications:
Gastric bypass surgery carries risks inherent to any surgical procedure, including bleeding, infection, blood clots, and adverse reactions to anaesthesia (1). The incidence of these complications is generally low, but it is essential to understand and address these potential risks with the surgical team.
Dumping syndrome:
Dumping syndrome is a common side effect of gastric bypass surgery, characterised by rapid emptying of the stomach contents into the small intestine. This can result in nausea, vomiting, abdominal cramps, diarrhoea, dizziness, and fatigue (2). Dietary modifications and eating patterns can help manage and minimise these symptoms.
Bowel obstruction:
In some cases, gastric bypass surgery may lead to bowel obstructions due to the formation of adhesions or internal hernias (3). Symptoms may include severe abdominal pain, vomiting, and the inability to pass gas or stool. Prompt medical attention is necessary if bowel obstruction is suspected.
Ulcers and strictures:
Gastric ulcers and strictures, which narrow the stomach or intestinal passages, can occur after gastric bypass surgery (4). These complications may lead to abdominal pain, nausea, vomiting, and difficulty swallowing. Medications, dietary modifications, and endoscopic interventions are commonly employed for treatment.
Psychological and social effects:
As discussed earlier in the article, it is essential to reiterate gastric bypass surgery’s potential psychological and social effects. Patients may experience psychological adjustment difficulties, body image concerns, and changes in social dynamics (5). Counselling, support groups, and ongoing psychological support are vital for addressing these effects.
Conclusion
Gastric bypass surgery offers a transformative approach to weight loss for individuals with obesity. However, as we have explored in this article, it is essential to consider the long-term effects and risks associated with this surgical intervention. While gastric bypass surgery can result in significant weight loss, improvements in metabolic parameters, and enhanced quality of life, it is not without potential complications and challenges.
Physiological standpoint
Physically, gastric bypass surgery impacts weight regulation, metabolic function, nutrient absorption, and gut microbiota. Long-term health risks may include nutritional deficiencies, metabolic syndrome, gastrointestinal complications, bone health issues, and potential effects on cardiovascular health (9). Additionally, there are psychological and emotional aspects to consider, such as body image concerns, the risk of developing eating disorders, and changes in mental health.
Factors influencing long-term Success
Factors influencing long-term Success include adherence to lifestyle changes, ongoing support, and individual characteristics. Preoperative and postoperative interventions and long-term follow-up care are crucial in optimising outcomes and addressing potential complications (10). It is imperative for healthcare professionals and patients to be aware of these effects and risks to make informed decisions, implement appropriate strategies, and provide comprehensive care.
By understanding gastric bypass surgery’s long-term effects and risks, individuals can navigate this weight loss journey with knowledge, support, and effective management strategies. Further research is necessary to continue improving outcomes and enhancing the overall well-being of patients who undergo this transformative procedure.
References
- Buchwald, H., Estok, R., Fahrbach, K., Banel, D., Jensen, M. D., Pories, W. J., … & Sledge, I. (2009). Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. The American Journal of Medicine, 122(3), 248-256. https://pubmed.ncbi.nlm.nih.gov/19272486/
- Adams, T. D., Gress, R. E., Smith, S. C., Halverson, R. C., Simper, S. C., Rosamond, W. D., … & Hunt, S. C. (2007). Long-term mortality after gastric bypass surgery. New England Journal of Medicine, 357(8), 753-761. https://pubmed.ncbi.nlm.nih.gov/17715409/
- Carlsson, L. M. S., Peltonen, M., Ahlin, S., Anveden, Å., Bouchard, C., Carlsson, B., … & Sjöholm, K. (2012). Bariatric surgery and prevention of type 2 diabetes in Swedish obese subjects. New England Journal of Medicine, 367(8), 695-704. https://pubmed.ncbi.nlm.nih.gov/22913680/
- Courcoulas, A. P., Christian, N. J., Belle, S. H., Berk, P. D., Flum, D. R., Garcia, L., … & Wolfe, B. M. (2013). Weight change and health outcomes three years after bariatric surgery among individuals with severe obesity. JAMA, 310(22), 2416-2425. https://pubmed.ncbi.nlm.nih.gov/24189773/
- Magro, D. O., Geloneze, B., Delfini, R., Pareja, B. C., Callejas, F., & Pareja, J. C. (2008). Long-term weight regains after gastric bypass: a 5-year prospective study. Obesity surgery, 18(6), 648-651. https://pubmed.ncbi.nlm.nih.gov/18392907/
- Adams, T. D., Gress, R. E., Smith, S. C., Halverson, R. C., Simper, S. C., Rosamond, W. D., … & Hunt, S. C. (2007). Long-term mortality after gastric bypass surgery. New England Journal of Medicine, 357(8), 753-761.
- Peterli, R., Wölnerhanssen, B. K., Peters, T., Vetter, D., Kröll, D., Borbély, Y., … & Beglinger, C. (2018). Improvement in glucose metabolism after bariatric surgery: comparison of laparoscopic Roux-en-Y gastric bypass and laparoscopic sleeve gastrectomy: a prospective randomized trial. Annals of Surgery, 267(5), 760-766.
- Schauer, P. R., Bhatt, D. L., Kirwan, J. P., Wolski, K., Brethauer, S. A., Navaneethan, S. D., … & Aminian, A. (2017). Bariatric surgery versus intensive medical therapy for diabetes—5-year outcomes. New England Journal of Medicine, 376(7), 641-651.
- Livhits, M., Mercado, C., Yermilov, I., Parikh, J. A., Dutson, E., Mehran, A., … & Gibbons, M. M. (2012). Preoperative predictors of weight loss following bariatric surgery: systematic review. Obesity Surgery, 22(1), 70-89.
- Livhits, M., Mercado, C., Yermilov, I., Parikh, J. A., Dutson, E., Mehran, A., … & Gibbons, M. M. (2012). Does weight loss immediately before bariatric surgery improve outcomes: a systematic review. Surgery for Obesity and Related Diseases, 8(6), 708-715.